 As a result, it became Medicare Part A B C D. Then, part C was added for private insurance companies. Later, medical coverage was added to the hospital coverage. Medicare started out as hospital insurance. You pay the premium directly to the private company and not to the government. Private companies providing this coverage are annually certified, and approved, by the Centers for Medicare & Medicaid Services. Part D is optional, requires a premium, and is offered through private companies. Anyone with Part A or B is eligible for Part D. It is the Medicare program which covers prescription drugs. Medicare Part D is last part of the Medicare part A B C D alphabet. MediGap insurance pays after Medicare pays. Medicare Advantage pays instead of Medicare. Whereas Part C includes Parts A and B, and can include extra coverage. The difference is that MediGap insurance is in addition to Medicare part A and B. Medicare Advantage is not Medicare Supplemental (MediGap) insurance. The insurer provides your benefits not the government. The difference between Part C and the combination of Part A and B, is that you pay the premium to private insurer. Part C plans with prescription drug benefits are known as “Medicare Advantage” (MA) plans. 
You can receive more coverage beyond parts A and B. Part C allows you to have your Medicare benefits administered through private health insurance plans. You now have the option to enroll in Medicare part C. The passage of the Balanced Budget Act of 1997 added C to Medicare part A B C D. There was a move in 1997 to “privatize” Medicare. Medicare Supplemental Insurance is only available if you are receiving benefits from Part A and B. You must go to a private insurance company to receive this coverage. There are different parts of Medicare: Part A covers inpatient hospital stays, care in a skilled nursing facility, hospice care, and some home health care. They are not sold or administered by the government. The MediGap plans are standardized by the government. This is the reason for Medicare Supplement Insurance (sometimes called MediGap). There are holes or “gaps” in the Medicare part A and B coverage. Medicare is a government national health insurance program in the United States, begun in 1965 under the Social Security Administration (SSA) and now administered by the Centers for Medicare and Medicaid Services (CMS). Medicare part A B C D does not cover everything. Otherwise, you will have to pay a premium to receive this coverage. If you are still working, your employer’s insurance may cover this part. Part B is optional and you must pay a premium. Physical therapy and some preventive screenings are also covered. Medicare Part B added coverage for medically necessary services. It did not cover medically necessary services like doctor’s services, diagnostic tests and outpatient care. There was a short coming in the original Medicare plan. Long-term or custodial care are not covered in any Medicare part A B C D. Part A does not cover long-term or custodial care. 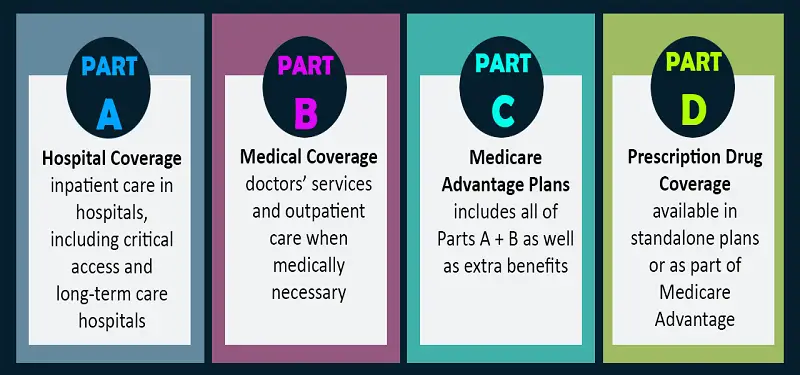
Most people do not have to pay a premium to get Part A. Today, home health care and hospice facility care are also included. The Parts of MedicareĮveryone who is eligible for Medicare receive Medicare Part A benefits automatically. Part A initially covered inpatient hospital care and skilled nursing facility care. If you were looking for Social Security A B C D, know that there is no Social Security A B C D, but Medicare Part ABCD. Medicare is strongly associated with Social Security. You also must meet minimum work amount requirements. You are eligible if you paid into social security during your working life. If the doctor or facility is out of network, you will pay a larger portion of your medical bill.With the enactment of the Medicare law, many people became eligible for Medicare. While there are many other features to an HMO, the main thing to know is that they use networks to manage care and costs.Ī PPO (Preferred Provider Organization) gives flexibility regarding the doctors you see and the health care facilities you use. This is because the provider is not in your Medicare HMO plan’s network. If you use an out-of-network provider, you will likely pay all of your medical bills, with the exception of emergency or urgent care visits. You will likely pay a lower rate for care. If you use an in-network doctor or hospital, it means the provider is approved by your plan. By looking at your specific circumstances, we will assist you in choosing the plan that is right for you, based on your individual needs and budget.Īn HMO (Health Maintenance Organization) features a network of approved doctors, hospitals, and other health care facilities. The two most popular are HMO and PPO plans. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
